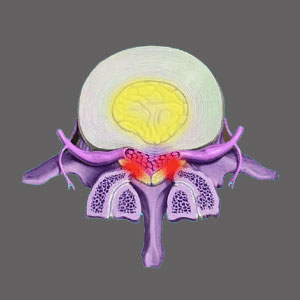
Degenerative spinal stenosis refers to central or foraminal narrowing which worsens with time and the continuing aging of the vertebral structures. Anatomical degeneration is a natural and normal part of getting older and is known to affect virtually all the tissues of the spine, including the bones, ligaments, intervertebral discs and neurological tissues. Being that there is no way to cure or reverse the majority of degenerative changes, most patients simply must accept that age may worsen the degree of stenotic changes they experience, but this does not mean that symptoms will escalate in every case. In fact, the degenerative changes in the vertebral column can actually help to ease some symptomatic expressions of stenosis in some specific circumstances.
This essay profiles how spinal stenosis can be caused, worsened or even relieved by spinal aging.
Degenerative Spinal Stenosis Contributors
Degeneration simply means the slow break down of anatomical tissues. It can also be called aging. We all know that time and activity cause virtually every part of our bodies to suffer some degree of deterioration. In some situations, there is observable physical evidence of this, while in other cases, there is functional evidence demonstrated in the activities we can no longer perform up to our former ability.
Let’s take a moment to review some of the degenerative processes which are normal to experience as we get older, yet may still cause of contribute to stenotic changes in the spine:
Disc desiccation is universal and is a known contributor to intervertebral herniation, as well as a facilitator of the osteoarthritic processes.
Herniated discs can cause acute or slow onset stenotic changes in the central canal or within the foraminal openings. The likelihood of intervertebral herniation increases with age and activity, due to typical changes inside the disc structures, particularly in the lower back and neck.
Osteoarthritis is a given for people past middle age and is usually found on many spinal structures. Osteophytes, osteochondral bars, and general arthritic debris can form on the facet joints, inside the central canal or within the neuroforamen. These factors are some of the most common direct causes of all types of spinal stenosis.
Ligament hypertrophy is not inherent to the aging processes, but is a common result. Ligament inflammation can contribute to various types of stenotic changes throughout the spine, but is usually a factor in cases of lumbar stenosis.
Spinal Degeneration Escalation
Being that aging and degeneration are continuous, some patients might expect to suffer an escalation of whatever types of stenosis currently affect them. Wear and tear will accumulate in degenerated areas of the spine, often worsening the degree of stenosis and further increasing the likelihood of neurological effects.
Minor arthritis, for example, will not likely cause any stenosis symptoms, but as the arthritic processes accumulate, the central or foraminal canals might become closed off to the extent of necessitating symptomatic expression.
The same can be said for a combination of soft tissue pathologies working together over time to narrow these same anatomical spaces, such as in the virtually universal scenario of disc disease, subsequent herniation and possible ligamentous hypertrophy.
While it is not sure that time and age will worsen stenosis, it is certainly possible and does occur in the majority of diagnosed patients.
Degenerative Spinal Stenosis Exceptions
There are some circumstances where the degenerative processes can actually assist in reducing the degree or expression of stenosis. While these do not represent the rule, they are not as rare as one might think and I have personally seen many instances in my decades of involvement in patient advocacy and chronic pain coaching work.
Acute herniated discs will often resolve with time, since the disc may dry out, reducing the extent of the annulus bulging and taking pressure off affected neurological tissues. This is one scenario where continuing disc desiccation or even rupture may be beneficial.
The arthritic processes can wear against one another, actually grinding down problematic bones spurs, especially near the facet joints. Some patients with diagnosed osteophytes will enjoy complete resolution of symptoms as the joints actually wear down the offending arthritic accumulations until the neuroforaminal openings become patent enough to relieve symptoms.
The body can also sometimes absorb small pieces of arthritic debris, as well as disc fragments, or these might migrate on their own to areas not affected by stenosis.
Spinal Stenosis > Spinal Stenosis Diagnosis > Degenerative Spinal Stenosis





